Foot and Ankle Specialist in Chanda Nagar
Ankle arthroscopy is keyhole surgery used to treat a variety of ankle problems. It is commonly used to treat and assess problems such as:
- Ankle bony ‘spurs’ (osteophytes).
- Loose bodies (chips of bone or cartilage).
- Arthritis.
- Cartilage or bone damage (osteochondral lesions).
- Scarring / ligament damage.
- ‘Impingement’ (anterior –front, or posterior-back of ankle).
- Small fractures.
- Used in combination with ligament repair/reconstruction surgery.
The surgery is performed as day case surgery. A general anaesthetic will usually be given and local anaesthetic is placed into the incisions to numb some of the pain following surgery.
Two or three ‘keyholes’ are made for small telescopes and instruments to see into the joint and ‘clean up’ or treat lesions.
The surgery usually takes between 45 minutes to one hour.
After surgery you will go home a few hours later once you have recovered. (You will need someone else to pick you up from hospital).
RECOVERY
Crutches are required for the first few days until it is comfortable to walk on your foot unaided.
Generally, ‘Full weight bearing’ as much as is comfortable is allowed – Occasionally you may be instructed by your surgeon to be ‘Non weight bearing’ (this is sometimes required following a ‘microfracture’ procedure).
Please REST and ELEVATE your foot strictly for the first 36-48 hours and then keep it mostly rested and elevated for the first week. Icing for 20 minutes twice or three times daily for the first 3-5 days can help with swelling and pain.
The outer soft bandage can be removed 48 hours after surgery and then an elastic ‘tubigrip’ applied to help control swelling. The stick-on plastic dressings should be left on until your review – if these fall off please replace with a bandaid. A small amount of bleeding on the dressings is normal.
The foot and ankle should be moved up and down and in circles to prevent stiffening and blood clots.
Physiotherapy may be started after 10 days if required. Stationary bike exercise can start 5-7 days post-op.
No driving right foot for 1 week or until walking comfortably with no crutches.
| Time Off Work | |
|---|---|
| Desk work | 4-7 days |
| Light duties | 1-2 weeks |
| Standing / heavy work | 3-5 weeks |
| Sports | 6-12 weeks |
| Full recovery | 3-4 months |
RISKS
The risks of arthroscopic ankle surgery are rare but include: Anaesthetic complications, Infection, Nerve damage, Blood clots (DVT) and Stiffness.
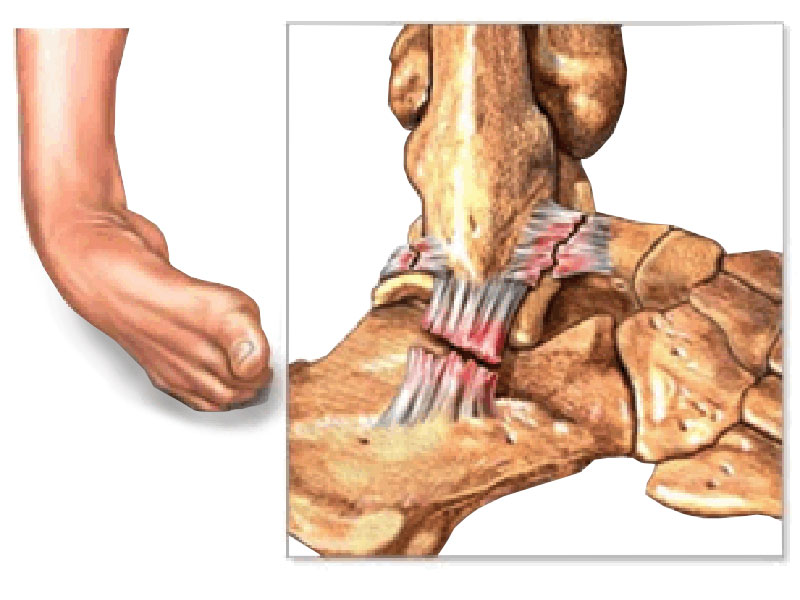
Ankle sprains are one of the most common sporting injuries. Usually the injury recovers with suitable rest and physiotherapy. Ankle instability occurs when the ankle repeatedly gives way during sporting or daily activities. This leads to recurrent ankle sprains, joint pain, swelling, inflammation, and further damage to the ligaments around the ankle. Some people experience intermittent ankle pain, which occur with episodes of instability, whilst others feel that their ankle aches more often. Recurrent instability episodes can cause damage to the joint surface cartilage, the formation of bony spurs (osteophytes), and arthritis.
NON-OPERATIVE MANAGEMENT
The first line of treatment for ankle sprains is rest, ice, compression, elevation with painkillers and anti-inflammatories (if tolerated). Physiotherapy is then useful to regain range of movement, strength, balance and joint position sense (proprioception). An ankle brace may be useful for people who have tried all these measures and experience ongoing problems with sporting or daily activities. Finally, a targeted PRP injection may offer relief from ankle inflammation and help settle symptoms so that physiotherapy can continue.
OPERATIVE MANAGEMENT
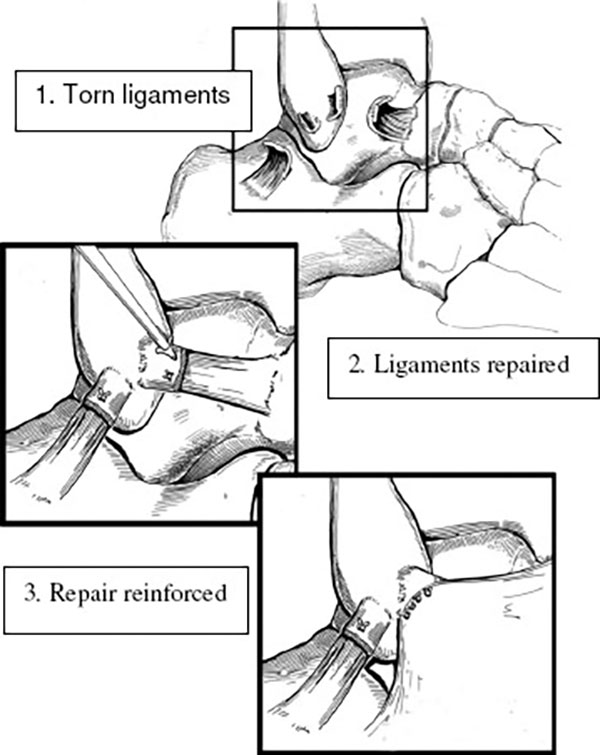
When all these non-operative measures fail, and recurrent ankle instability becomes an ongoing problem, surgery is indicated. The ankle ligaments are assessed clinically and an MRI scan may be necessary to identify any problems within the ankle joint itself or the tendons and ligaments around the joint. There are 2 components to the surgery. An incision is made over the outside of the ankle where the ligaments have been torn away and the ligaments are reconstructed in an anatomical fashion and reinforced with overlying tissue (modified Bröstrum-Gould repair). If indicated, the tendons behind the ankle are inspected and repaired. At the end of the operation a backslab (half plaster) is applied to immobilise the ankle and protect the reconstruction and wounds.
In addition to the ligament repair, an arthroscopy is initially performed through 2 small incisions at the front of the ankle. The joint surfaces are inspected, inflammatory and scar tissue is removed, and any bony spurs (osteophytes) are trimmed away.
POST-OPERATIVE RECOVERY
As with all reconstructive surgery your rehabilitation and postoperative physiotherapy regime forms a vital part of your recovery from surgery and return to normal activities. The first 2 weeks are dedicated to reducing the swelling with elevation of the foot and mobilising non-weight bearing with crutches to allow the wounds to heal. You will then be allowed to wear a lace up ankle brace and gradually increase your weight bearing status and work on range of motion. 6 weeks after surgery the brace is removed for daily activities and an intensive strengthening and balance program begins. The brace is to be worn for all sporting activities and you should be able to return to sport 3-6 months after surgery. The ankle may always be a bit stiffer than the normal side, but this is rarely a significant problem.
RISKS AND COMPLICATIONS
No surgery is completely risk free. The risks and complications will be assessed and discussed with you. There is always a small risk of infection, blood clots, nerve injury and anaesthetic problems and measures are taken to reduce these. There is approximately a 5% chance of experiencing problems with recurrent instability and this is usually due to a fresh injury or sprain. A good outcome is achieved in more than 90% of cases.
| Recovery Times | |
|---|---|
| Hospital stay | 1 night |
| Rest & elevation | 7-10 days |
| Plaster = crutches (non-weight bearing) | 2 weeks |
| Lace-up brace/cam walker (full time – 2 weeks partial then 2 weeks full weight bearing) | 4 weeks |
| Lace-up brace (training) | 6 weeks |
| Ankle strapping (competition) | 12+ weeks |
| Time off Work | |
|---|---|
| Seated | 2-3 weeks |
| Standing | 6 weeks |
| Heavy Physical Work | 12 weeks |
Following surgery, a formal recovery protocol will be given to you to pass on to your physiotherapist.
Ankle replacement surgery is an option for end stage ankle arthritis. This may have been discussed with you or planned for your ankle arthritis problem.
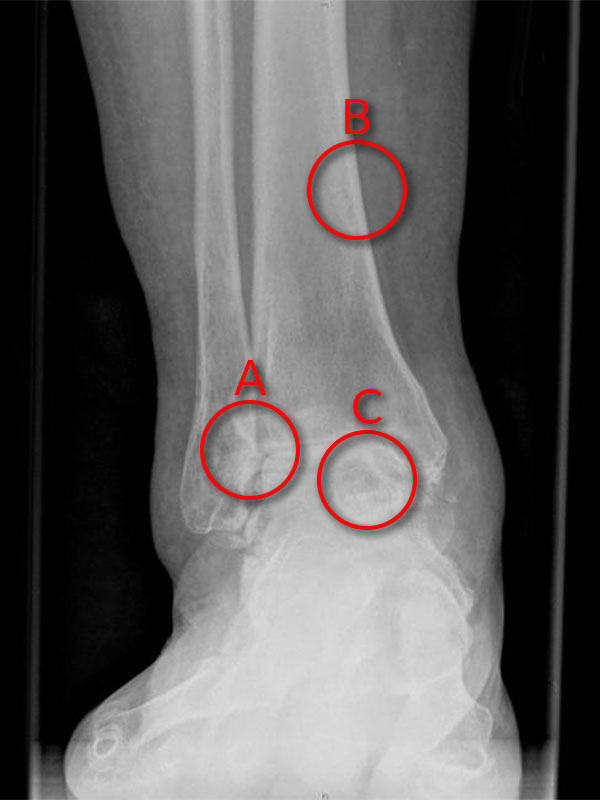
(A: Loss of cartilage in joint space – ‘bone on bone’ arthritis, B: Tibia, C: Talus.)
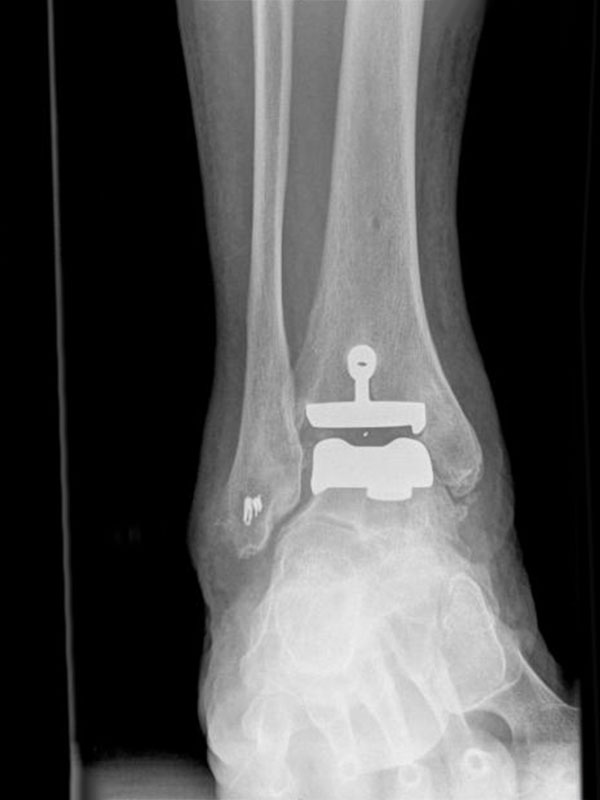
One recent study showed that people with end stage ankle arthritis suffer just as much pain and disability as people with end stage hip arthritis (not surprising really).
Ankle replacement technology has been improving over recent years. The original ankle replacements performed over 30 years ago were not very successful. Newer technology and experience in ankle replacements has meant over the last 10 years newer designs have had improved results.
Ankle replacements are still uncommon and ankle arthritis is 20 times less common than hip or knee arthritis. Therefore not many people have heard of ankle replacements and usually you will not have heard of ‘someone who has had one done’ – compared to hips and knees. The current replacements are having good results although still not quite as good as hip and knee replacements.
Overall approximately 80% (8 out of 10) ankles will last for more than 10 years without any major problems. As with any artificial joint they can wear out, become loose or infected. Care must be taken not to over stress the joint as this may lead to premature wear. However, regular day-to-day activities such as walking, golf, swimming, snow skiing and bike riding should be possible. Running is usually not possible and not encouraged (Except to get out of the way of an oncoming car)!
A small percentage of ankles will have minor troubles such as scar tissue impingement or early wear of the plastic liner that may need minor adjustment surgery within the first few years.
Of the 10-20% that may wear out over 5-10 years then the main option is to remove the ankle and then fuse the ankle joint. Occasionally a ‘redo’ or revision of the ankle prosthesis may be possible.

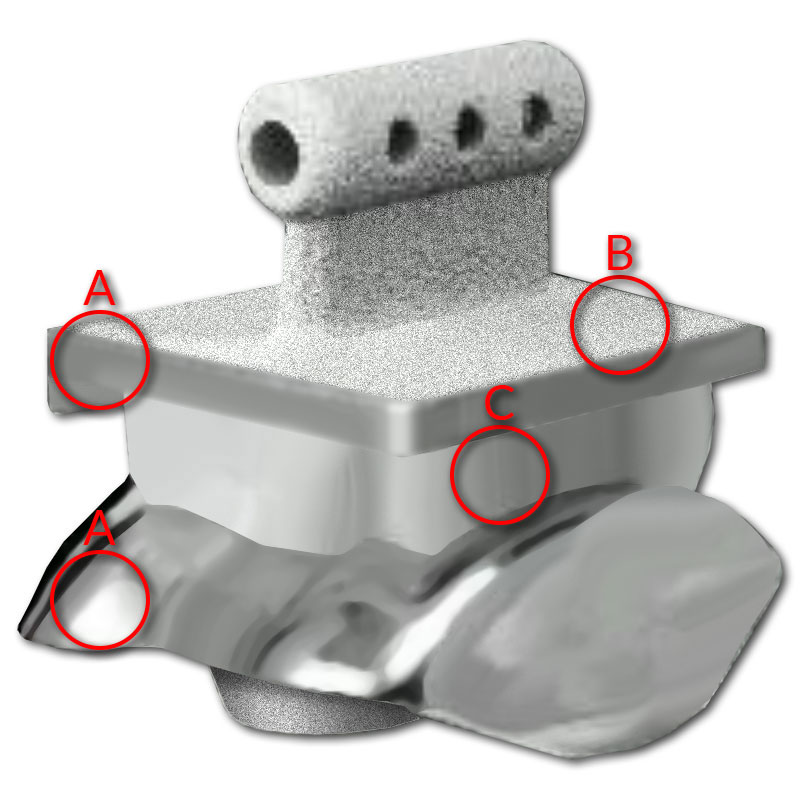
(A: Metallic components – tibia and talus, B: Roughened surface allows bone attachment, C: Articulating plastic (polyethylene) component.)
Pain relief is the main aim of any ankle arthritis surgery and an ankle replacement will generally give good to excellent relief of pain (equivalent to an ankle fusion). Sometimes there may be an occasional ‘niggle’ as it is an artificial joint with moving parts and not ‘normal’.
The advantage of an ankle replacement is the ability to maintain movement in the joint. This encourages a more normal walking gait pattern and therefore better functional outcome. It also helps ‘protect’ the surrounding joints (e.g. subtalar joint) compared to an ankle fusion. With an ankle fusion the surrounding joints have to ‘work harder’ after the surgery and may have progressive arthritis, which requires fusion of more joints in the foot (not ideal). An ankle replacement will not allow full normal movement but certainly gives a good useable range of movement.
Overall most people are very happy with their ankle replacement and get back to a relatively active lifestyle without the severe pain of ankle arthritis.
SURGERY
The surgery is done generally under general anaesthesia or spinal anaesthetic. The operation takes approximately 2 hours.
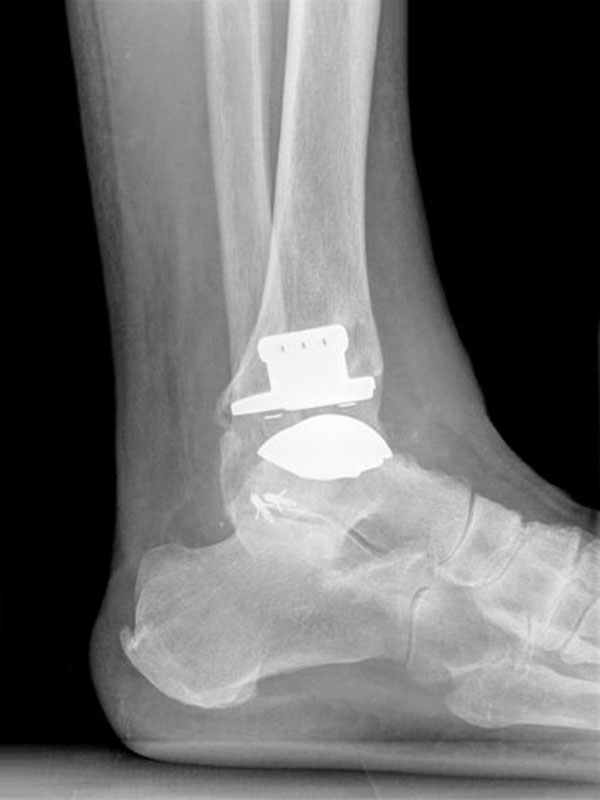
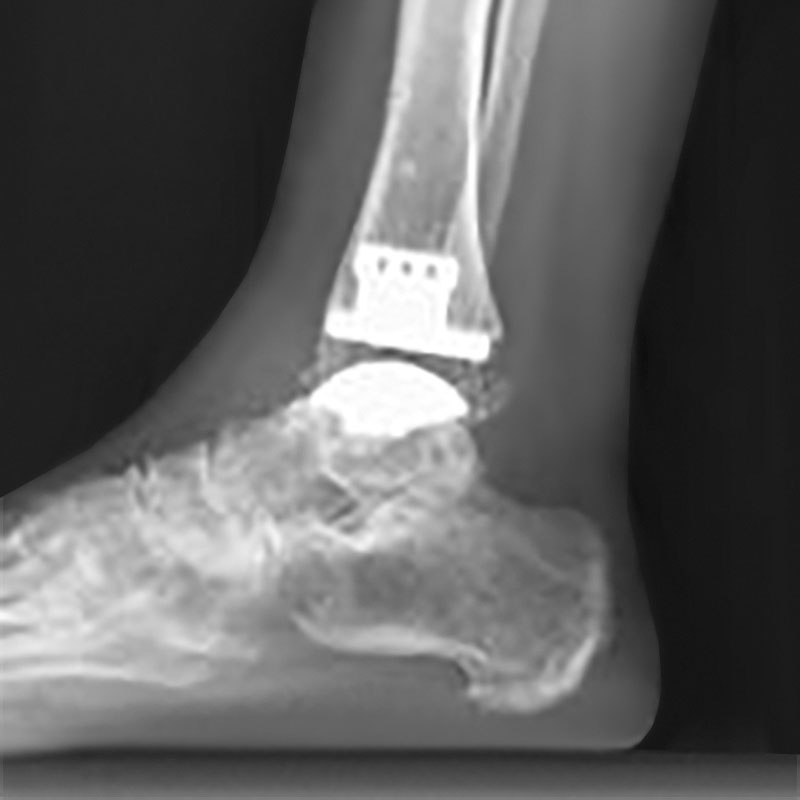
An incision is made over the front of the ankle. The worn out surfaces of the ankle joint are carefully resected and special instruments are used to help guide the insertion of the prosthesis. There is a metal component (made of titanium and chrome cobalt) on the bottom of the shin bone (tibia) and one on the top of the ankle bone (talus), in between these is an articulating biocompatible plastic (polyethylene).
The components are ‘uncemented’ – meaning they have a roughened surface that allows the bone to slowly grow onto the prosthesis so that it becomes permanently fixed to your bone.
Occasionally other procedures are required at the same time to lengthen a tight Achilles tendon, stabilise ligaments or realign / fuse surrounding bones or joints. When you wake up your leg will be in a plaster splint. An anaesthetic nerve block is usually placed into your leg during surgery to help reduce pain after surgery.
RECOVERY
Usually 3-4 days are spent in hospital until pain has subsided and you have learnt to hop on crutches or a frame.
The first 2 weeks at home are spent with the leg elevated recovering from surgery. This is critical to minimise swelling and give the wound the best chance of healing well.
After 2 weeks the cast and sutures are removed. You then may be placed into a moon boot or further cast depending on your surgery.
At 6 weeks full weight bearing is usually allowed and physiotherapy begun. Your moon boot may still be required for some support for a few more weeks.
By 2-3 months you will be walking well. It is not uncommon to have some ‘inflammation’ phase around 3 months –this will generally settle.
More full recovery of swelling, strength and general comfort in your ankle will take 6+ months.
RISKS
Possible risks of the surgery include: Anaesthetic risks, infection, fracture, DVT (blood clots), nerve damage, bleeding/ bruising, stiffness, scarring, loosening of the replacement, pain, failure of the prosthesis and need for further surgery.
| Recovery Times | |
|---|---|
| Hospital stay | 1 night |
| Rest & elevation | 7-10 days |
| Plaster = crutches (non-weight bearing) | 2 weeks |
| Lace-up brace/cam walker (full time – 2 weeks partial then 2 weeks full weight bearing) | 4 weeks |
| Lace-up brace (training) | 6 weeks |
| Ankle strapping (competition) | 12+ weeks |
| Time off Work | |
|---|---|
| Seated | 2-3 weeks |
| Standing | 6 weeks |
| Heavy Physical Work | 12 weeks |
Foot and ankle surgery is a specialised area of orthopaedic surgery. The surgery can be quite challenging and every patient is different with unique needs and goals.
You will need to follow instructions, perform appropriate exercises, and modify your activities during your healing process.
This requires patience, persistence, and a desire to get better. If you are unable to complete the post-operative instructions it will affect your results and you should consider alternative treatments.
Successful results from surgery require a contribution from you.
Foot and ankle surgery is a specialized field of orthopedics that deals with surgical interventions for conditions related to the feet and ankles, such as fractures, arthritis, and ligament injuries. The goal of foot and ankle surgery is to alleviate pain, improve function, and restore mobility for patients with foot and ankle conditions.
It is important that you read all of the information carefully. The information provided is intended to be a guide and not all-inclusive. If you have any questions, concerns, or are not certain about the benefits, risks, limitations, or alternatives to your treatment, please do not hesitate to ask your surgeon.
PREPARING FOR SURGERY
- On the morning of surgery please shower and thoroughly wash your feet and toes with soap (anti-bacterial if available) and water.
- Fast from the time instructed.
- On the day of surgery do NOT take any Insulin or diabetes tablets unless otherwise instructed. (If you are normally on Insulin please confirm with us that we have this information). Aspirin and any blood thinners (e.g. warfarin, Plavix, Iscover) should have been stopped one week before surgery.
- Otherwise please take your normal medications (e.g., blood pressure tablets) with a small sip of water.
- Attend hospital at appropriate time – there may be some waiting time before your surgery but you need to arrive so that you can be checked in by the nursing staff and seen by the anaesthetist beforehand. Please bring a book, magazine or music in case of a moderate wait or delay.
- Remember to bring your X-rays / Scans please.
PAIN MANAGEMENT
A local anaesthetic block may be given to you during surgery. This will produce numbness around the nerves in the region of your surgical procedure. It will provide you with pain relief for approximately 12-18 hours post-operatively, enabling you to be comfortable and allow sleep after your surgery. It will also allow time to take some of your oral painkillers prior to the block wearing off and prevent a sudden onset of pain.
It is best to take your painkillers regularly for the first 1-2 weeks. Initially, prescription medication is usually necessary and after the initial 2-3 days, regular Panadol or Panadeine is usually all that is required.
It is also worthwhile taking painkillers prior to your first post-operative visit to ensure that plaster and suture removal is more comfortable.
Remember, pain is better managed if you get on top of it before it gets on top of you.
DRESSINGS AND EXTERNAL PINS
- Please leave your bandages intact until reviewed by your surgeon at the postoperative visit (except for ankle scopes and plantar fascia release where the outer bandage can be removed after 2 days). A plastic garbage/kitchen bag sealed with tape and elastic band +-‘glad wrap’ is needed to keep it dry in the shower or bath. If there is excessive bleeding leaking through the bandage or the bandages get wet please contact the rooms and this can easily be re-bandaged if required.
- Rest and elevation of your foot (to at least the level of your hip and ideally above the level of your heart) is required for the first 10 days following surgery. This helps minimise swelling and aids healing of your wounds.
- Icing of the area (if possible) for 20 minutes 2-3 times per day for the first 3-5 days can also help reduce swelling and pain.
- If part of your wound continues to ooze, this usually only requires regular dressing changes. If you have any concerns, please contact the rooms prior to commencing any antibiotics.
- Similarly, if the pins used to straighten your toes are knocked, it is unusual to do any damage. However if the toe becomes deformed or there is prolonged pain then contact the rooms.
- Gentle leg, ankle, foot and toe movement and stretching (if possible and not in plaster) every hour will help with circulation and muscle recovery.
- If you have been instructed to be ‘non-weight bearing’ this is to allow best healing of bones/tendons/ligaments.Failure to comply may jeopardise the results of your surgery.
- Time off work and recovery will depend on the nature of your surgery. Generally a minimum of one to two weeks is required off for seated/ deskwork (unless very minor surgery). For more prolonged standing or walking this will often require at least 4-6 weeks (or longer).
- A ’post-op’ appointment will be made 2 weeks after surgery for removal of stitches and to check the healing of your wounds. The next follow up will usually be a further 4-6 weeks later to check further recovery.
- If physiotherapy is required this will be arranged/ discussed at your follow up appointment.
SWELLING
Swelling often increases over the first 6 weeks and then usually reduces over the next 6 weeks. Depending on the nature and magnitude of the surgery, it may take up to 12 months to fully settle. This is the normal way the body heals. Rest and elevation is helpful. As the foot swells it is common to have stiffness and mild nerve pain so attention to swelling is important.
EXERCISE
However, do not overdo it. Too much too early can be just as bad as not doing enough. This includes sport. Your surgeon is happy to liaise with your trainers to get you back on the field as quickly as possible without compromising your recovery process and long-term health.
COMPLICATIONS
Fortunately complications are uncommon. Nevertheless they do occur and you need to be aware of them. The following is a non-exhaustive list of some of the more frequent. You should also be aware that several factors can increase your chance of having a complication. These include smoking, diabetes, and obesity. You can reduce this risk by quitting smoking, good blood sugar control, and losing weight.
INFECTION
This occurs when the wound is invaded by bacteria, usually from your surrounding skin. Signs you may have an infection include heat, tenderness, unusual fluid, or an odour coming from your wound. You may also have a fever or feel generally unwell. Most infections can be treated with antibiotics but more serious ones require admission to hospital and further surgery to clean out the wound.
WOUND HEALING
Normal wound healing requires adequate blood flow and active healing cells. Being too active early after surgery causes bleeding and swelling which can cause part of the wound to open. The foot is very delicate in this respect. It is important that you rest and keep your foot elevated as much as possible for the first 7-10 days to encourage healing and discourage wound break down. Risks of infection and healing problems are much higher if you smoke or are diabetic. If you are able to give up smoking before and for a few weeks after your surgery this will help your healing process.
NERVES
Nerves are the electrical system of the body. It is extremely rare for nerves to be cut but nerves are commonly affected by swelling after surgery. This can cause partial numbness and sometimes burning pain. This generally resolves as the swelling subsides. In rare cases this can persist.
STIFFNESS
Both injury and surgery create scar tissue. Some people are prone to develop excess scar tissue. When this is combined with post-operative swelling it may lead to joint stiffness. Most of this can be addressed through good quality rehabilitation techniques and your own involvement in recovery.
BONE HEALING
Surgeons can only create the environment for bone healing. It is your body that performs the final joining process. This can fail if there is too much mobility (i.e. you walk on it too early) or if there are other issues such as smoking, blood flow problems or infection. If the bone fails to heal it may require further surgery.
DEEP VEIN THROMBOSIS (DVT) AND PULMONARY EMBOLISM (PE)
These fortunately are very rare events but can have serious consequences. Signs you may have a DVT include swelling that is not reduced with elevation of the leg, colour changes or coldness of the toes, calf pain or tenderness. Signs you may have a PE include chest pain or shortness of breath. Seek immediate medical attention if you are concerned.
PROLONGED OR EXCESSIVE PAIN
This can be a sign of a variety of complications following surgery, with many mentioned previously. On very rare occasions a chronic regional pain syndrome can develop in addition to these and require further prolonged management.
ANAESTHETIC (GENERAL, SPINAL, NERVE BLOCKS)
Any concerns should be discussed with your anaesthetist during the pre-operative consultation.
After surgery you should notify your surgeon / GP / Emergency department if you have any of the following:
- Increasing pain (despite painkillers, rest elevation and icing).
- Increasing swelling (despite rest and elevation above the level of your heart).
- Fevers or sweats.
- Discharge or increasing redness of your wound.
- Shortness of breath or chest pains.
- Persistent numbness (greater than 48hrs after surgery).
For most surgeries it takes a minimum of 3 months to be recovering reasonably well (75%), 6 months until 90% recovered and 12 months until complete recovery. Swelling is normal for the first 3-4 months and can take 6-12 months before full recovery is expected.
Hallux rigidus (HR) refers to stiffness (rigidus) of the joint at the base of the great toe (hallux). This joint is called the great toe metatarsophalangeal joint (MTPJ). The usual cause of HR is arthritis or wear and tear of the smooth cartilage that lines the joint. HR may be caused by a previous injury or it may be part of a general medical condition e.g. gout. Often the cause is unknown; it just develops, particularly as people get older.
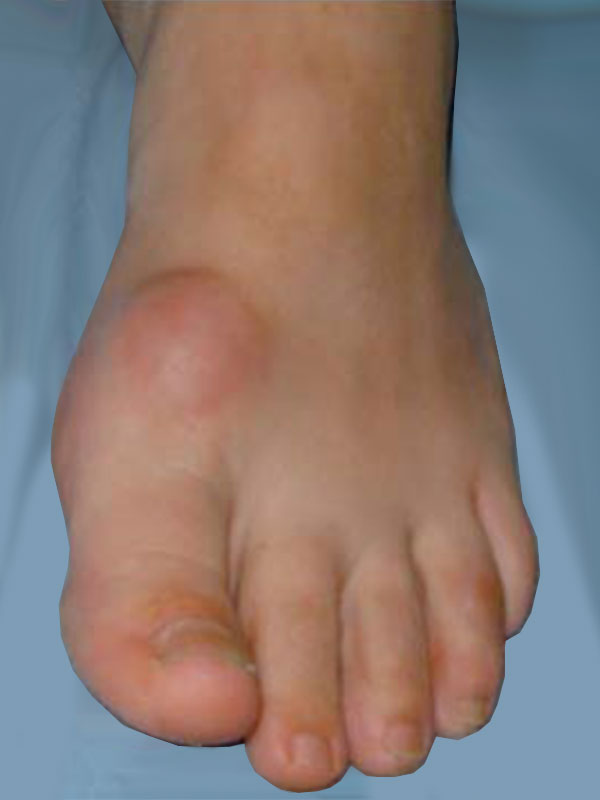
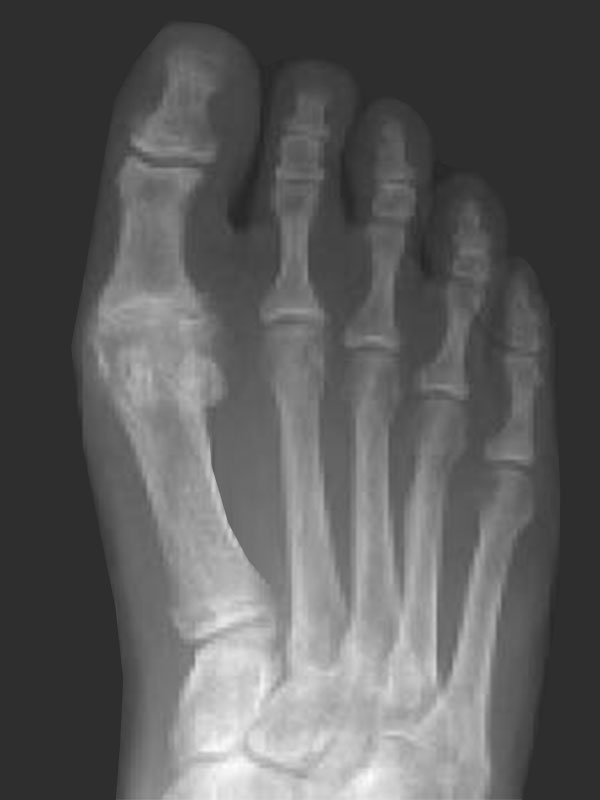
HR presents with stiffness and pain in the great toe MTPJ. If the symptoms are severe, it may limit walking distance, and compromise work and recreational activities. Bony spurs (osteophytes) develop around the great toe MTPJ and can cause pain by rubbing against tight fitting shoes. In an attempt to off-load the painful great toe, some people will preferentially walk on the outer border of the foot, causing transfer pain to the lesser toes.
NON-OPERATIVE MANAGEMENT
The main aims are to relieve pain and decrease loading and movement through the great toe MTPJ. In it’s mildest form, HR may not need operative treatment. Simple lifestyle and activity modifications including weight loss, the use of a walking aids and the avoidance of high impact activities may be all that is necessary. In addition, taking painkillers (Panadol and anti-inflammatories), and wearing appropriate shoe wear and orthotics (stiff insoles or shoes with a rocker bottom) can all be helpful. High heels and shoes with a narrow toe box should be avoided. Finally, a cortisone injection may offer relief of inflammation but as with most treatments, the degree and extent of relief varies from patient to patient.
OPERATIVE MANAGEMENT
Surgery is considered when the previous measures fail. There are two main surgical options to relieve pain and improve quality of life. The first option includes motion-preserving procedures such as joint debridement +/-osteotomy, and the alternative is an arthrodesis or fusion of the MTPJ. The best option for an individual patient depends on many factors including the severity of arthritis, the age and functional demands of the patient, and the presence of arthritis in adjacent joints. The final choice is a joint decision between surgeon and patient.
MTPJ DEBRIDEMENT +/-OSTEOTOMY
If the HR is mild, affecting only the upper part of the joint, this upper portion may be trimmed and the joint washed out. This is often combined with a realignment procedure (Moberg osteotomy) of the bone at the base of the great toe (proximal phalynx). More recently, this has become possible using a minimally invasive technique. This allows the use of smaller incisions and generally results in a more rapid recovery and an improved cosmetic result.
In more advanced cases, the joint debridement may be combined with resection of part of the proximal phalynx and the insertion of some of the surrounding soft tissue into the resulting cavity (Hamilton-Thompson Interposition Arthroplasty). This combination can provide long lasting pain relief with improved movement of the great toe in the appropriate patient.
In around 20% of patients who have undergone either of these procedures, the arthritis is progressive and symptoms may return to a point where further procedures such as joint fusion may be required.
MTPJ REPLACEMENT
Artificial joints that replace the surfaces of the diseased bone (in a similar fashion to hip and knee replacements) have been used to treat advanced arthritis. However, previous implants have shown poor results and any subsequent procedures (such as fusion) have become more difficult.
The current generation of implants appear to show more promising results but as yet, long-term reliability has not been established and for this reason, your surgeon does not currently recommend or perform this procedure.
MTPJ ARTHRODESIS (FUSION)
This is the ‘gold standard’ procedure for moderate to severe arthritis. The remaining cartilage in the joint is removed, the bones on either side of the joint are fused together and held with screws in isolation or a combination of screws and a plate. 90-95% of patients will experience good pain relief with this. However, the joint is stiffened and this limits the wearing of high heels and makes running difficult. There is a small risk of developing arthritis in the next joint along the big toe but this is rarely troublesome.
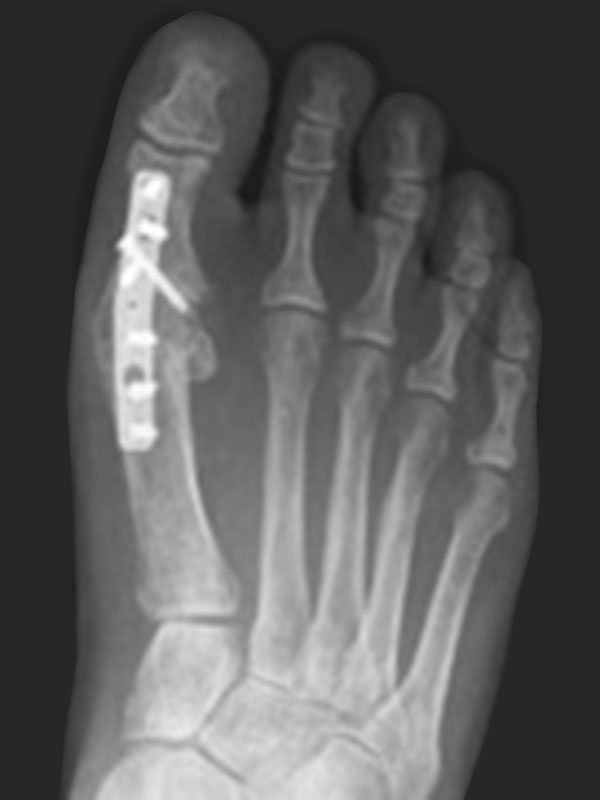
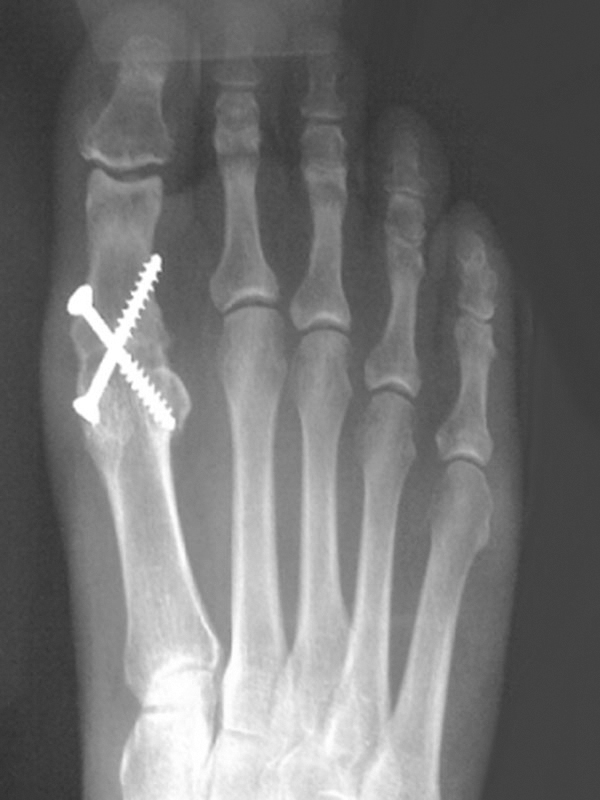
COMPLICATIONS
Less than 5-10% will develop a complication that may require further intervention. These include wound-healing problems, infection, damage to nerves and blood vessels, incomplete relief of symptoms, and in the case of arthrodesis, failure of the bones to knit together requiring further surgery.
| Recovery Times | |
|---|---|
| Hospital stay | 1 night |
| Rest & elevation | 10 days |
| Crutches / Frame | 1-2 weeks |
| Foot swelling | 12 weeks |
| Shoes | |
|---|---|
| Hospital (Fusion) | 6 weeks |
| Hospital (Debridement) | 4-6 weeks |
| Wide | 6-12 weeks |
| Normal | 12 weeks |
| Fashionable | Up to 6 Months |
| Time off Work | |
|---|---|
| Time off Work(Seated) | 3-4 weeks |
| Time off Work(Standing) | 6-8 weeks |
| Result Times (pain relief & function) | |
|---|---|
| Good | 3 months |
| Better | 6 months |
| Best | 12 months |
This brochure is a brief overview of the surgical management of hallux rigidus and not designed to be all-inclusive. If you have any further questions, please do not hesitate to contact your surgeon.
Bunions are a common deformity in the community. They are thought to occur due to a muscle imbalance that is often inherited. Inappropriate footwear may exacerbate the condition however is not usually the underlying cause. Bunions worsen with advancing age and can eventually cause pain and deformity. The bunion may also result in damage to other parts of your feet. Pain is felt because of their size and abnormal biomechanics. The time to have treatment is when they cause significant pain or you have difficulty in finding comfortable footwear.
NON-OPERATIVE MANAGEMENT
The operative treatment of bunion correction that is utilized by your surgeon is the Scarf and Akin osteotomy. Many operations for bunions have been tried over the years with varying levels of success. Most have failed due to high recurrence rates, excessive joint stiffness, or by transferring problems to other parts of the foot. The Scarf / Akin osteotomy solves many of these problems. The procedure has been popularised by Mr Louis Barouk (French orthopaedic foot surgeon) and it is the most common style of bunion operation performed in Europe. The keys to its success are that it is restores foot mechanics, allows early return of joint motion, and has low recurrence rates.
The procedure has 5 components performed through 2 incisions. Initially, one of the tight ligaments and the tight muscle on the opposite side of the bunion is released. The bunion is then shaved. The metatarsal bone is cut and adjusted to narrow the foot and realign the joint. This is called a Scarf osteotomy, and 2 small screws are placed in the bone to provide solid fixation. After this a wedge of bone is removed from the phalanx bone to straighten the big toe. This is the Akin osteotomy, and a small staple or screw is used to hold the bone in place. The joint capsule is finally tightened where the bunion has stretched it and the skin is closed. The metalwork usually does not need to be removed.
Before
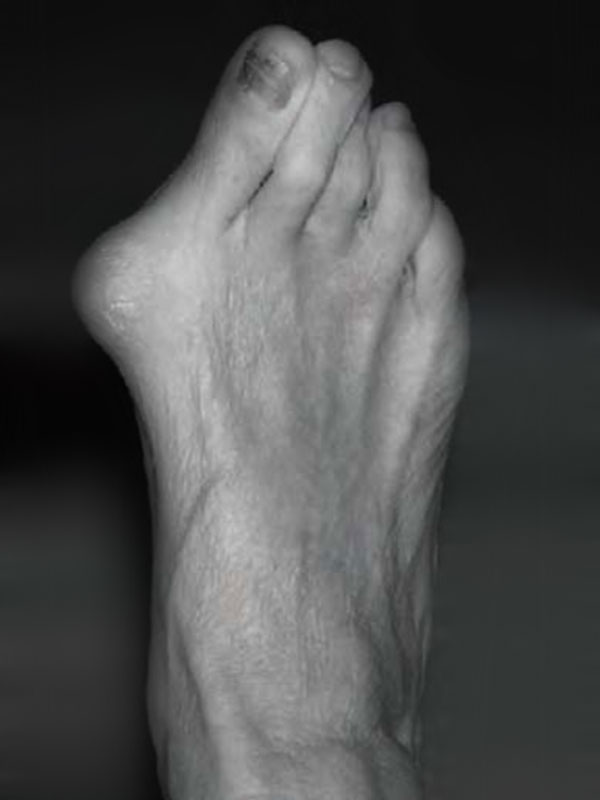
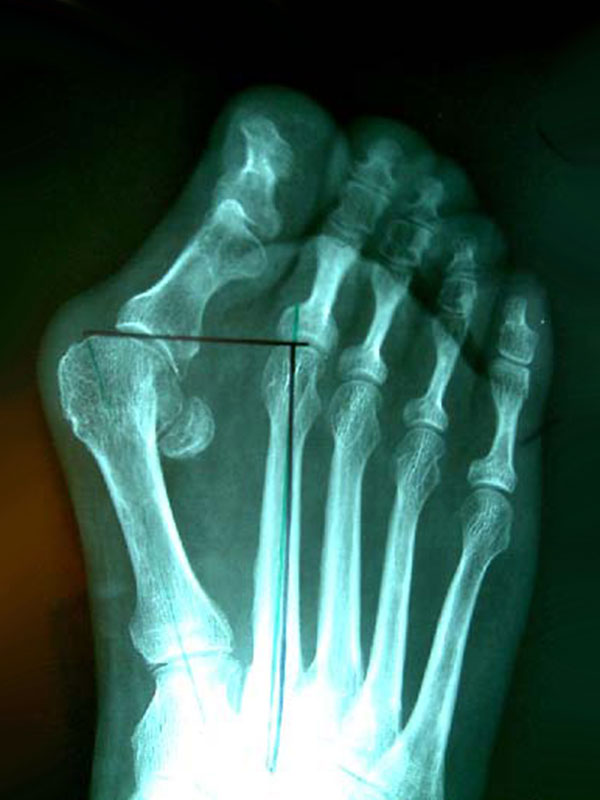
More recently, this procedure has become possible for may patients using a minimally invasive technique. This allows the use of smaller incisions (usually 5 or 6 incisions around 3-5mm in length) and generally results in a slightly more rapid recovery and an improved cosmetic result. As the underlying bony procedure is almost identical to that of the open technique, the longer-term results are very similar
After
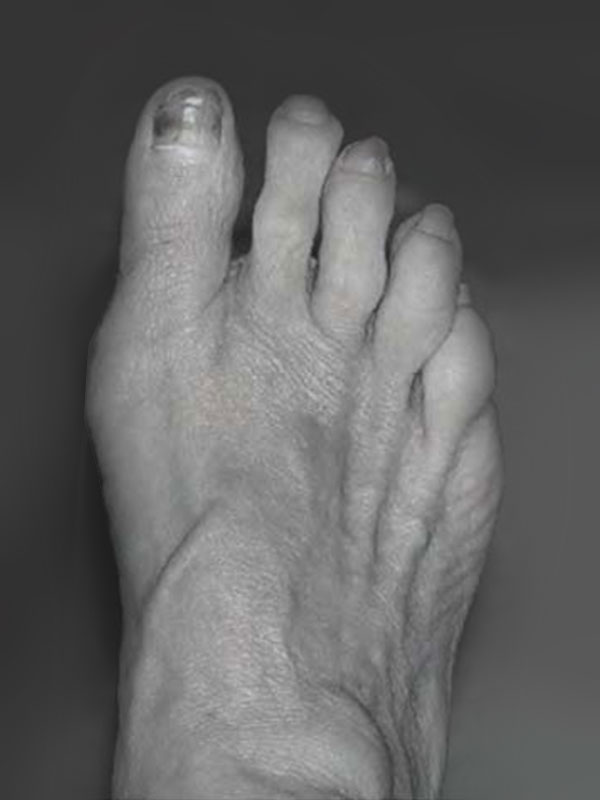
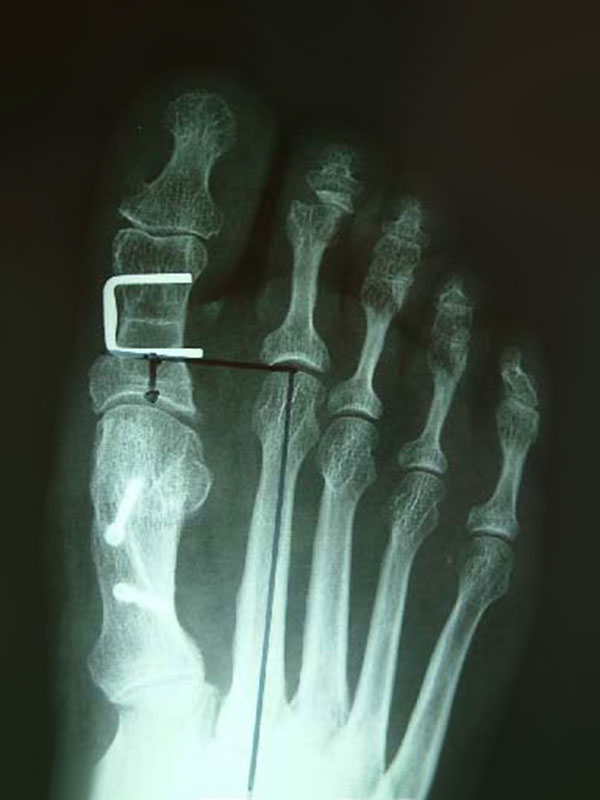
POST-OPERATIVE MANAGEMENT
mmediate weight bearing is possible in a postoperative stiff soled shoe and plaster is not required. The way your foot has been bandaged assists in holding the big toe in place, with the post-operative shoe protecting the toe when you walk. This takes the place of a plaster and accordingly is required for between 4 and 6 weeks. As with all foot surgery, swelling occurs and this is the main limitation to activity and footwear in the early stages. Swelling often increases over a 6-week period and then reduces over a further 6 weeks. As such your final result will begin 3 months after surgery. As the mechanics in your foot have been substantially changed, your body will go on making subtle adjustments over a 12-month period.
Foot surgery without appropriate pain relief is extremely uncomfortable. While the operation is performed under general anaesthetic, a nerve block is also usually inserted, which puts the foot to sleep for around 12-18 hours. You should wake up from surgery with minimal pain and it is now uncommon for injectable pain relief to be required. When the block wears off you can take simple oral pain relief. It is important to start taking your oral pain relief prior to the block wearing off as once the pain becomes intense, it can become difficult to manage.
COMPLICATIONS
No surgery is risk free. The risks and complications will be assessed and discussed with you. There is always a small risk of infection, blood clots and anaesthetic problems with lower limb surgery and measures are taken to reduce these. In bunion surgery there is also a 5% chance of recurrence of the deformity, overcorrection of the big toe, or problems with bone fixation. Very rarely, the toe can become numb or hypersensitive for a prolonged period. Conversely, a successful outcome is achieved in more than 90% of patients.
| Recovery Times | |
|---|---|
| Hospital stay | 1 night |
| Rest & elevation | 10 days |
| Crutches / Frame | 1-2 weeks |
| Foot swelling | 12 weeks |
| Shoes | |
|---|---|
| Hospital | < 6 weeks |
| Wide | 6-12 weeks |
| Normal | 12 weeks |
| Fashionable | Up to 6 Months |
| Time off Work | |
|---|---|
| Seated | 3-4 weeks |
| Standing | 6-8 weeks |
| Lifting / Carrying | 8-12 weeks |
This brochure is a brief overview of the surgical management of hallux rigidus and not designed to be all-inclusive. If you have any further questions, please do not hesitate to contact your surgeon.
Lesser toe deformities can cause problems in a variety of ways. ‘Hammer’ or ‘claw‘ toes are the most common toe deformities that require surgical treatment. They can cause problems relating to the prominent knuckle joint (PIP joint) on the toe sticking up and rubbing on shoe-wear and causing corn formation and ulcers. The deformity of the toe may cause pain itself from inflammation in the main joint (MTP joint) at the base of the toe or damage and stretching of the ligament under the toe and ball of the foot. Sometimes the toe deformity causes extra pressure under the ‘ball’ of the foot with a feeling of pain or even a sensation of walking on a ‘pebble’.
CAUSES OF ‘HAMMER’ TOE DEFORMITIES
The cause of these problems can be multifactorial:
- Genetic factors.
- Tight shoe-wear.
- Presence of a ‘bunion’.
- Neurological causes.
- Rheumatoid or other types of arthritis.
- The particular anatomy of your foot (e.g. long second toe).
- Overuse and ligament damage.
NON-OPERATIVE MANAGEMENT
Non-surgical methods of treatment should always be considered first before any surgery. This can involve things such as:
- Appropriate shoewear with a ‘roomy’ toebox on your shoe (wide and deep).
- Orthotics / insoles – may be an option for pain under the ‘ball’ of your foot.
- Taping or strapping of your toe for early hammer toes or ligament damage.
- Silicone sleeves or soft padding over the toe available from chemists or podiatrist/ orthotist.
If these measures fail to work or are unsatisfactory then surgery can be performed to straighten the toe.
OPERATIVE MANAGEMENT
Surgery can involve a number of small procedures on the toe depending on the degree of deformity and the exact problem.
Usually the bent knuckle in the middle of the toe (the PIP joint) will need to be straightened and possibly fused. This may require a pin in the toe which is left just 5mm out of the toe. This will then be removed after 4-6 weeks. Removal of the pin is straight forward. It takes just a few seconds and is no more painful than having stitches removed. No anaesthetic is required. Sometimes an internal pin or dissolvable pin can be used without the need for an external pin.
Other adjustments such as lengthening tight tendons or shortening the Metatarsal head (knuckle bone at bottom of toe joint) – which is called a ‘Weil osteotomy’ –may also be required.
Surgery is generally performed as day surgery unless combined with bunion or other surgery, which may require an overnight stay.
Weight bearing is allowed in a post-operative sandal. Elevation for at least the first 5-7 days is important. Reasonable recovery occurs by 4-5 weeks once the bones are healing. The toe can remain swollen for up to 3 months but will recover.
Some stiffness of the toe is common as the toe cannot be made perfect again once the previous damage has already occurred. The toe however should be straighter and more comfortable.
The plantar fascia runs along the length of the sole of the foot and along with various ligaments and muscles of the foot, functions to assist in maintaining its inner arch (like the string of a bow, with the bones of the foot being the bow itself).
Plantar fasciitis is an inflammation of the origin of the fascia at the calcaneus (heel bone). It is a result of a repetitive strain / tear and repair of the fascia from traction forces that have worn it out. It can be likened to an elastic band that has been left out in the sun and stretched too many times; it loses its stretch and has many micro-tears in it.
Heel spurs have long been associated with heel pain, and were originally thought to be its cause. Heel spurs occur at the origin of the flexor digitorum brevis muscle, which lies just beneath the plantar fascia. However, heel spurs are NOT the cause of heel pain associated with plantar fasciitis and for this reason, it is unnecessary for them to be removed. They probably form because of the local inflammation in the soft tissue, with the body forming bone mistakenly in its attempt to repair the plantar fascia.
NON-OPERATIVE MANAGEMENT
Initial management of plantar fasciitis involves a multi-modal non-operative approach. For 90% of people, this is all that is required. This initially includes analgesics, anti-inflammatories, massage, applying ice, and exercises that stretch the fascia and strengthen the muscles. Orthoses including cushioning heel pads and night splints may also be helpful, along with corticosteroid or PRP injections, and other alternative modalities such as ultrasound or shock wave therapy.
OPERATIVE MANAGEMENT
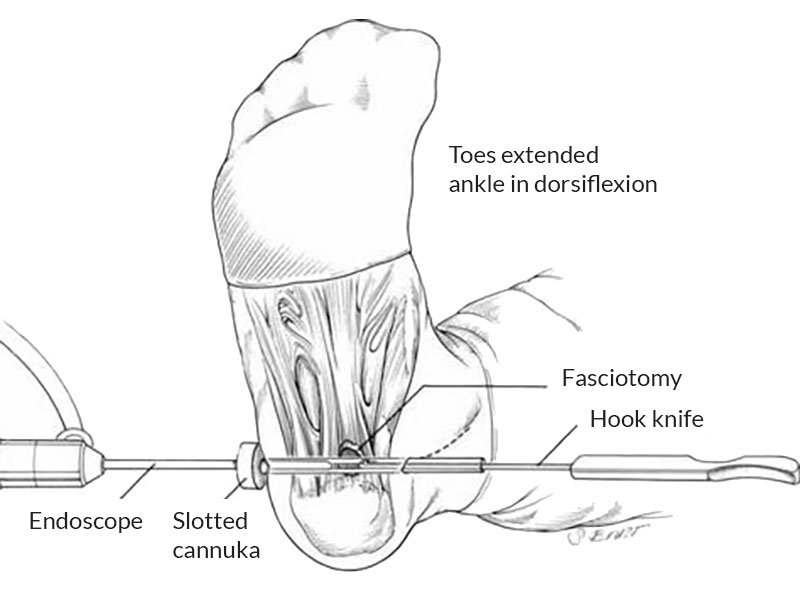
For those patients who have ongoing pain despite adequate non-operative management, operative intervention may be required. Conventionally this procedure has been performed through a large incision on the in-step of the foot. In recent times an endoscopic technique has been developed.
Our recent study of over 100 patients comparing the results of the traditional open procedure with the more modern endoscopic technique demonstrated the endoscopic procedure to be superior. This included improved patient satisfaction, less post-operative pain, quicker recovery times, and a lower complication rate.
The procedure involves making 2 x 10mm incisions; 1 on each side of the foot. This enables a telescopic camera and instrumentation to be inserted to complete the release of the plantar fascia. Patients are then allowed to weight bear as tolerated, and quite often have less pain than prior to the procedure within 1-2 weeks. By 4 weeks, patients are usually walking well, and may commence returning to sport by 6-12 weeks.
COMPLICATIONS
Complications are rare with this procedure. There is always a small risk of infection, nerve injury and blood clots, and anaesthetic problems with lower limb surgery and measures are taken to minimize these risks. A small proportion of patients may also experience a persistence of their preoperative pain despite surgery.
Finally, and uncommonly, discomfort in the outer part of the top of the foot may occur following any technique of plantar fascia release. Very seldom is this enough of a problem to require further surgery and generally improves with the use of insoles (orthotics). Overall, a successful outcome is achieved in approximately 90% of patients.
| Recovery Times | |
|---|---|
| Hospital stay | 1 night |
| Rest & elevation | 10 days |
| Crutches / Frame | 1-2 weeks |
| Foot swelling | 12 weeks |
| Sport | 6-12 weeks |
| Time off Work | |
|---|---|
| Seated | 1 weeks |
| Standing | 3-4 weeks |
This brochure is a brief overview of the surgical management of plantar fasciitis and not designed to be all-inclusive. If you have any further questions, please do not hesitate to contact your surgeon.
Frequently Asked Questions
The word arthritis literally means “joint inflammation.” Arthritis refers to a group of more than 100 rheumatic diseases and other conditions that cause pain, stiffness, and swelling in joints.
Rheumatoid arthritis is a disease that damages the lining surrounding our joints while also destroying our bones, tissue, and joints over time.
Osteoarthritis is a progressive condition that slowly damages the cartilage surrounding the ends of bones and is common in the hip, knee, and spine.
Arthroscopic surgery is a surgical procedure that is commonly performed to diagnose and treat problems within the joint. By using high-tech cameras, the orthopedic surgeon inserts a small instrument, called an arthroscope, into the joint.
The arthroscope contains a fiber optic light source and small television camera that allow the surgeon to view the joint on a television monitor and diagnose the problem, determine the extent of injury, and make any necessary repairs.
Joint replacement surgery is a surgical procedure that is performed to replace an arthritic or damaged joint with a new, artificial joint, called a prosthesis. Joint replacements can be performed on every joint in the body, but most commonly performed in the knee, hip, shoulder, and elbow.
Joints contain cartilage, a soft, rubbery gel-like coating on the ends of bones, where they articulate, that protects joints and facilitates movement and over time, or if the joint has been injured, the cartilage wears away and the bones of the joint start rubbing together. As the bones rub together, bone spurs may form, and the joint becomes stiff and painful. Most people have joint replacement surgery when they can no longer control the pain with medication and other treatments and the pain is significantly interfering with their lives.
